Top 10 Best Orthopedic Implants Plates You Should Know?
When discussing orthopedic implants plates, it is essential to understand their significant role in modern medicine. These plates stabilize bones during recovery and promote healing after fractures or surgeries. They come in various shapes and materials, each designed for specific needs. Surgeons use these orthopedic implants plates based on the patient's condition and the nature of the injury.
In today's healthcare landscape, miscommunication around these devices can occur. Not all implants are suitable for every patient. Sometimes, choosing the wrong plate can lead to complications. Patients must engage with their healthcare providers about the options available. This conversation can clarify doubts and lead to better outcomes.
Exploring the top 10 best orthopedic implants plates reveals a variety of innovative solutions. Some plates are lightweight yet strong, while others focus on flexibility. Each design has pros and cons, requiring careful consideration. As medical technology advances, the choice becomes even more complex. Understanding these products is vital for patients and healthcare professionals alike.
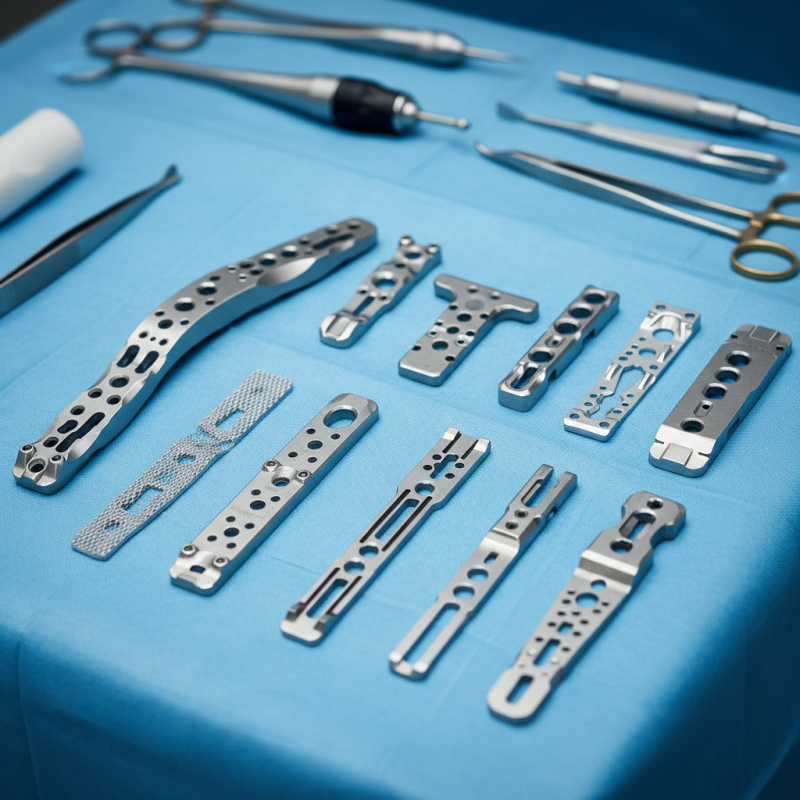
Top 10 Orthopedic Implant Plates: An Overview of Their Importance
Orthopedic implant plates play a crucial role in the healing process of bone fractures. These plates stabilize broken bones, allowing them to mend properly. According to recent industry reports, the orthopedic implant market is projected to reach over $70 billion by 2027, emphasizing their growing importance in healthcare.
Using these implants can significantly enhance recovery times. Studies show that proper stabilization leads to quicker healing, reducing hospital stays. However, the selection of the right plate is not always straightforward. Surgeons must consider factors like material, size, and specific patient needs. In certain cases, complications arise. Plate failures can occur due to poor alignment or patient non-compliance with post-operative care.
Additionally, there are environmental concerns associated with the production of these implants. The sourcing of materials and manufacturing processes can have significant ecological impacts. More sustainable practices are needed in the industry. Awareness and advancements in technology could lead to better, more eco-friendly implant options without compromising patient care. This balance is vital as the market continues to expand.
Top 10 Best Orthopedic Implants Plates
Material Composition of Orthopedic Plates: Titanium vs. Stainless Steel
When it comes to orthopedic plates, understanding material composition is crucial. Titanium and stainless steel are the two primary materials used. Each has unique properties that influence their performance in the body.
Titanium is lightweight and offers excellent corrosion resistance. It's known for its biocompatibility, making it a favorite among surgeons. Many believe it integrates well with bone.
However, stainless steel has its advantages too. It is often less expensive and has greater strength. This can be beneficial in high-stress scenarios. Yet, stainless steel is heavier, which may affect comfort. Infections can occur with both materials, highlighting the need for careful surgical techniques.
Surgeons must weigh these factors. They should consider each patient's unique needs and any potential complications. There is no one-size-fits-all solution. The ongoing debate about which material is superior can lead to uncertainty. This needs thoughtful reflection in the medical community. Choices made today will affect long-term recovery for patients.
Analyzing Load-Bearing Capacity in Orthopedic Implant Plates
When considering orthopedic implant plates, it's essential to analyze load-bearing capacity. Each plate must support specific weights during recovery. Understanding material strength is crucial. Different alloys may influence durability and performance.
Tips: Look for plates made from biocompatible materials. These can enhance healing and minimize complications. Always consult with a healthcare professional when choosing an implant.
The load-bearing capacity impacts mobility directly. A plate that can withstand stress ensures stabilization. However, not all implants fit every patient. Individual anatomy plays a vital role. This variability can lead to underperformance if overlooked.
Tips: Review case studies on load-bearing tests. They often provide practical insights. Think about your unique requirements when selecting an implant plate.
Innovative Technologies in Plate Design: Advancements in Biocompatibility

Advancements in orthopedic implants have revolutionized patient care. Innovative technologies in plate design focus on improving biocompatibility. This means the materials used are less likely to cause adverse reactions in the body.
Modern plates are designed with materials that mimic bone properties. They support healing while reducing inflammation. New surface treatments enhance integration with bone tissues. Understanding these technologies helps surgeons choose the best options for each patient.
Tip: Always consult with medical professionals about the latest implant options. Researching can help clarify questions.
Despite these advancements, challenges remain. Not all patients respond the same way. There can be issues with implant rejection or infection. Asking the right questions during consultations is crucial.
Tip: Consider speaking with others who have undergone similar procedures. Their insights can provide valuable perspectives on recovery and choices.
Clinical Outcomes and Success Rates of Common Orthopedic Plates
Orthopedic plates play a crucial role in stabilizing fractures and promoting healing. Clinical outcomes vary greatly among different types of plates. Success rates often depend on patient factors, surgical technique, and plate design. Many studies show that plates improve fracture alignment. However, complications can arise, including infections and non-unions. Not all patients respond positively to the same type of plate.
In clinical practice, outcomes are often mixed. Some patients report quick recovery with well-placed plates. Others experience prolonged healing times despite seemingly ideal conditions. Surgeon experience also affects results. An experienced surgeon may produce better outcomes. Still, the inherent variability in healing is a reminder that orthopedic solutions are not foolproof. Even the best-designed plates can't guarantee success for every individual.
Careful consideration is essential when choosing an orthopedic plate. Factors such as patient's age, activity level, and fracture type must be addressed. While many plates have proven effective, there is no universal solution. Ongoing research continues to explore innovations in this field. Feedback from both surgeons and patients can drive improvements. Understanding these elements helps in making informed decisions about treatment. The journey of recovery often needs patience and perseverance.
Top 10 Best Orthopedic Implants Plates You Should Know
| Plate Type | Material | Indications | Success Rate | Common Use |
|---|---|---|---|---|
| Locking Compression Plate (LCP) | Titanium/ Stainless Steel | Fractures, Osteotomies | 95% | Orthopedic Trauma |
| Dynamic Compression Plate (DCP) | Stainless Steel | Long Bone Fractures | 90% | General Fracture Repair |
| Tension Band Wiring | Stainless Steel | Patella Fractures | 85% | Knee Injuries |
| Polyaxial Locking Plate | Titanium Alloy | Complex Fractures | 92% | Trauma Surgery |
| Humeral Locking Plate | Stainless Steel | Humeral Fractures | 93% | Upper Limb Surgery |
| Craniofacial Plate | Titanium | Craniofacial Reconstruction | 88% | Facial Trauma |
| Elbow Locking Plate | Stainless Steel | Elbow Fractures | 92% | Upper Extremity Repairs |
| Ankle Locking Plate | Titanium | Ankle Fractures | 91% | Foot and Ankle Surgery |
| Thoracic Plate | Titanium/ Stainless Steel | Rib Fractures | 89% | Chest Trauma |
Related Posts
-

Orthopedic Plates and Screws Tips for Better Healing
-
2026 Best Orthopedic Surgical Instruments for Precision and Efficiency?
-
2026 Top Orthopedic Surgical Instruments You Need to Know?
-
Top Surgical Instruments Tips for Beginners to Enhance Skills?
-

How to Choose the Best Implant Surgical Instruments for Your Practice?
-
Top 10 Best Orthopedic Bone Screws for Effective Fracture Healing?
